What is Acne?
Acne is a skin condition that occurs when the pores in your skin become clogged with oil and dead skin cells. This can cause blackheads, whiteheads, pimples, and other types of blemishes. Acne can occur on any part of your body, but it is most common on the face, neck, chest, and back.

What Causes Acne?
There is no one definitive answer to this question. Acne can be caused by a variety of things, including genetics, hormones, stress, and Certain medications. However, the most common cause of acne is over-active sebaceous glands. These are the glands that secrete oil into your pores.
How Do You Get Rid of Acne?
Acne skin is irritated and overproduces sebum. Combined with bacteria in the pores, this leads to acne pustules. You need a gentle, acne-focused skincare regime to cleanse, soothe and protect the inflamed skin. BHA/Salicylic acid can then be used to reduce pore congestion and sebum overproduction.
What is Cystic Acne?
Cystic acne is a more severe form of acne that occurs when the pores in your skin become clogged with oil and dead skin cells. This can cause blackheads, whiteheads, pimples, and other types of blemishes. Cystic acne can be most common on the face, neck, chest, and back.
What Does Cystic Acne Look Like?
Cystic acne is a more severe form of acne that can cause large, red, and painful bumps on the skin. These bumps may also be filled with pus. Cystic acne can occur on any part of your body, but it is most commonly found on the face, neck, chest, and back.

What Causes Cystic Acne?
Cystic Acne can occur when bacteria, dead skin cells, and oil get trapped in your pores. This can cause your pores to become inflamed and can lead to the formation of pimples, blackheads, and whiteheads. Cystic acne is more common in people who have oily skin.
What is Fungal Acne?
What Causes Fungal Acne?
What Does Fungal Acne Look Like?
What Causes Chin Acne?
How to Get Rid of Acne Dark Spots?
How to heal acne scars?
How long does acne last?

How Do You Get Rid of Acne Scabs?
What causes acne in adults?
At what age does acne typically appear?
How long does it take for acne scars to fade?
Acne scars can take anywhere from a few weeks to a few months to fade. The best way to speed up the process is to use a natural scar treatment, such as vitamin E or aloe vera. You can also try using a derma roller or light therapy to reduce acne scaring.
How to treat acne scars?
Acne scars can take anywhere from two to eight weeks to fade. However, some people may see results in as little as two weeks, while others may need up to eight weeks.
How to treat hormonal acne naturally?
There are a few things you can do to treat hormonal acne naturally. First, try to reduce the amount of stress in your life. Second, eat a healthy diet and avoid processed foods. Third, wash your face twice a day with a gentle cleanser. Fourth, use a natural acne treatment, such as tea tree oil, to spot treat blemishes.
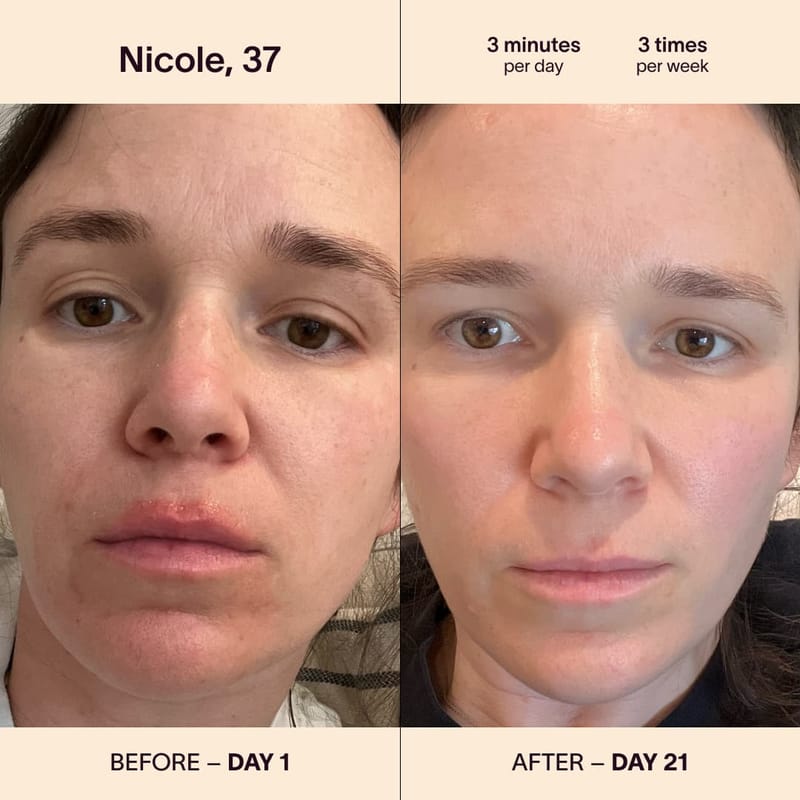
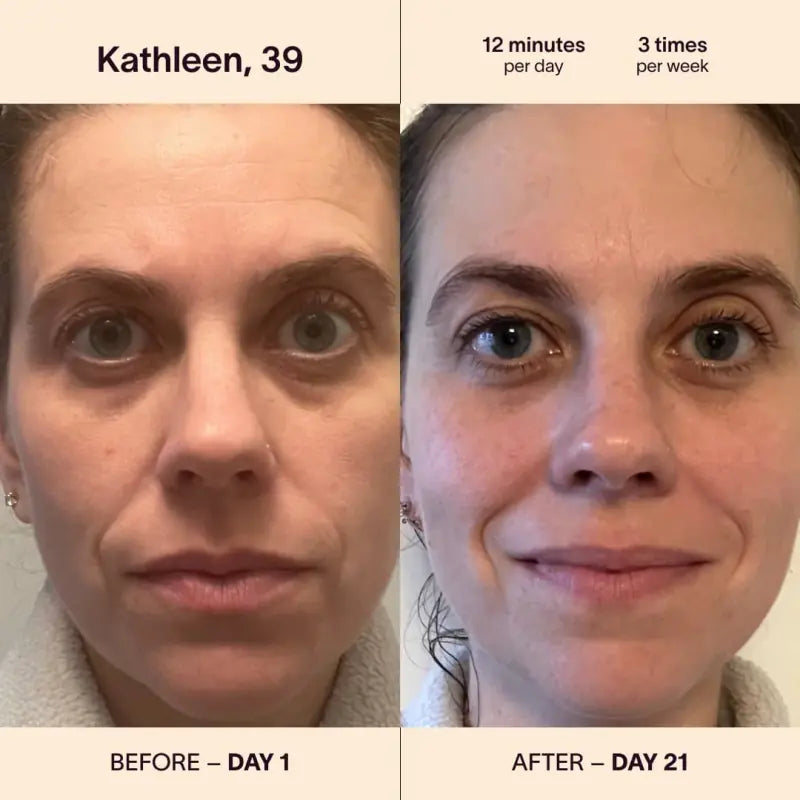
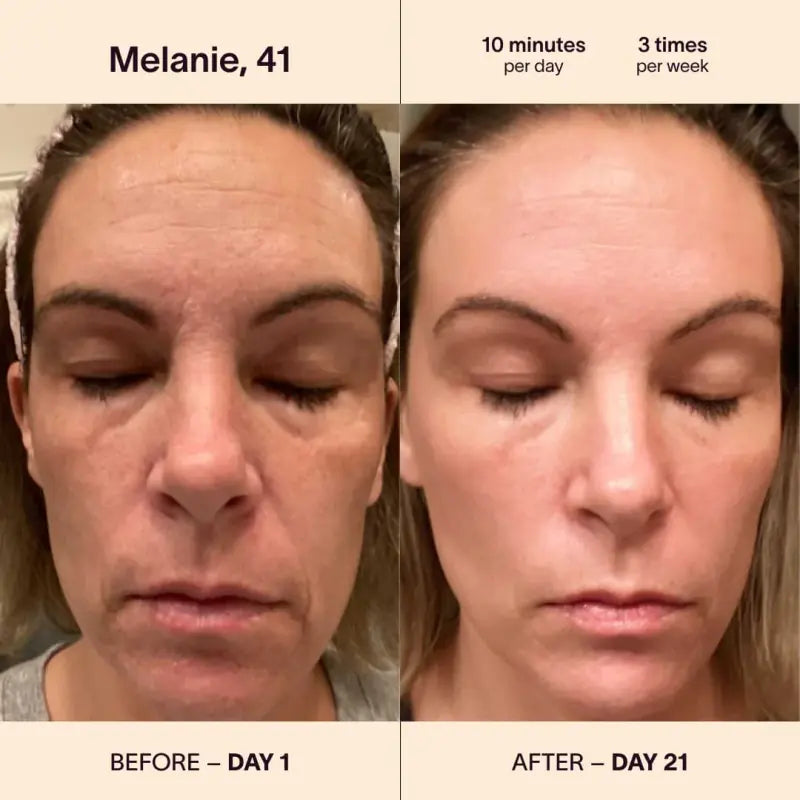
Can Red Light Therapy Wands Help Acne-Prone Skin?
Red light therapy wands have shown promise in reducing acne inflammation and promoting healing. The therapy works by stimulating collagen production and reducing the activity of oil glands. While results vary, many individuals with acne-prone skin have reported improvements in their condition. However, it is essential to consult a dermatologist for personalized advice.
Can Blue Light Therapy Prevent Future Breakouts?
Yes, blue light therapy has the potential to prevent future breakouts. It works by killing acne-causing bacteria on the skin and reducing inflammation. Regular treatments can help keep the skin clear and minimize the occurrence of acne. However, individual results may vary, and it's important to consult with a dermatologist for personalized advice and treatment options.
How Does Blue Light Therapy Work on Acne?
Blue light therapy works on acne by targeting the bacteria responsible for acne breakouts, specifically Propionibacterium acnes. The blue light activates a photosensitive compound within the bacteria, leading to the production of reactive oxygen species that destroy the bacteria. This therapy reduces inflammation and helps clear existing acne while preventing future outbreaks.
Can Blue Light Therapy Be Used Alongside Other Acne Treatments?
Yes, blue light therapy can be used alongside other acne treatments. It is often combined with topical medications, such as benzoyl peroxide or retinoids, to enhance their effectiveness. Blue light therapy can complement other treatments by targeting acne-causing bacteria while additional therapies address other aspects of acne, such as inflammation or excessive oil production.
Can Blue Light Therapy Help with Acne Scars?
Blue light therapy is primarily effective in targeting and killing acne-causing bacteria. While it may help reduce active acne and prevent new breakouts, its ability to directly address acne scars is limited. For treating acne scars, other modalities such as laser resurfacing, chemical peels, or microneedling may be more suitable options.
Can Stress Trigger Acne Breakouts?
Yes, stress can trigger acne breakouts. When stressed, the body releases hormones like cortisol, which can increase oil production and inflammation in the skin, leading to clogged pores and acne flare-ups. Maintaining a balanced lifestyle and managing stress can help minimize the impact on skin health.
What Role Does Hydration Play In Acne Prevention?
Hydration helps maintain healthy skin by supporting cell function and regeneration. Adequate water intake can flush toxins from your body, preventing pore clogging and acne. Moisturized skin also reduces oil production, a leading acne cause. Therefore, staying hydrated is crucial in maintaining clear skin and reducing the likelihood of acne breakouts.
How Often Should I Cleanse My Skin To Prevent Acne?
To prevent acne, cleanse your skin twice daily. Over-cleansing can strip natural oils, leading to dryness and irritation. Use a mild, non-comedogenic cleanser and follow with a moisturizer suitable for your skin type. Consistent cleansing helps remove excess oil, dirt, and impurities, promoting healthier and clearer skin.
Is It Possible To Prevent Acne With Natural Remedies?
Yes, it is possible to prevent acne with natural remedies. A healthy diet, proper skincare, tea tree oil, aloe vera, and green tea are some natural options that can help control acne. However, results may vary, and consulting a dermatologist is recommended for severe cases.
How Does Sleep Affect The Likelihood Of Acne Breakouts?
Sleep can significantly impact acne breakouts. Inadequate sleep can elevate stress hormones, leading to increased inflammation and sebum production, exacerbating acne. Moreover, sleep deprivation weakens the immune system's ability to combat bacteria, making the skin more susceptible to outbreaks. Prioritizing quality sleep can help improve overall skin health and reduce acne breakouts.
Can Stress Cause Fungal Acne?
Stress can exacerbate fungal acne by disrupting the immune system and hormonal balance, which can increase oil production on the skin. This excess oil can provide a breeding ground for the yeast that causes fungal acne, thereby potentially worsening the condition. Stress management techniques may help reduce outbreaks.
Can Fungal Acne Leave Scars?
Fungal acne typically does not leave scars. However, if the skin condition leads to intense inflammation or is aggravated by scratching or improper treatment, there can be post-inflammatory hyperpigmentation or superficial scarring. Proper treatment and resisting the urge to pick or scratch are important to prevent any skin damage.
Can Hormones Affect Fungal Acne?
Hormonal fluctuations can affect fungal acne by increasing sebum production, creating an ideal environment for the overgrowth of Malassezia yeast responsible for the condition. Particularly during puberty, menstruation, pregnancy, or when using oral contraceptives, hormonal changes may exacerbate or trigger fungal acne flare-ups.
Can Makeup Worsen Fungal Acne?
Makeup can exacerbate fungal acne if it's occlusive, trapping moisture and creating an environment where fungi thrive. Oil-based products are particularly problematic. Non-comedogenic, fungal-acne safe products are better choices. Always remove makeup thoroughly and maintain a clean makeup routine to mitigate worsening of fungal acne.
What Causes Acne-Prone Skin?
Acne-prone skin is primarily caused by overproduction of sebum, clogged pores, inflammation, and bacteria. Hormonal imbalances, particularly during puberty, can exacerbate sebum production. External factors like diet, stress, and certain skincare products can also contribute. Genetics play a role in skin's susceptibility to acne.
Can Dairy Intake Affect Acne-Prone Skin?
Yes, dairy intake can affect acne-prone skin. Dairy products, particularly skim milk, have hormones that may stimulate oil glands in the skin, leading to increased sebum production and potentially worsening acne. The link varies among individuals, with some more sensitive to dairy's effects on their skin condition.
Can Stress Trigger Breakouts in Acne-Prone Skin?
Yes, stress can trigger breakouts in acne-prone skin. Stress increases cortisol production, which can stimulate oil glands to produce more sebum, leading to clogged pores and acne. Stress also may affect the skin's barrier function, making it more susceptible to acne-causing bacteria and inflammation.
How Often Should Acne-Prone Skin Be Moisturized?
Acne-prone skin should be moisturized daily, ideally twice a day after cleansing. Using a lightweight, non-comedogenic moisturizer prevents over-drying and irritation, which can exacerbate acne. It's important to maintain skin hydration balance to help regulate oil production and support the skin's natural barrier function.
Are There Natural Remedies for Acne-Prone Skin?
Yes, natural remedies for acne-prone skin include tea tree oil, known for its antibacterial properties; green tea extract, reducing inflammation and sebum production; aloe vera, soothing skin and reducing redness; and honey, with antimicrobial qualities. These can be applied topically, complementing traditional acne treatments for improved skin health.
Can Over-Cleansing Worsen Acne-Prone Skin?
Yes, over-cleansing can worsen acne-prone skin. Excessive washing strips the skin of its natural oils, leading to overproduction of sebum, which can clog pores and exacerbate acne. It also disrupts the skin's pH balance and barrier function, making it more susceptible to irritation and inflammation.
What Ingredients Should Be Avoided in Acne-Prone Skin Products?
For acne-prone skin, avoid ingredients like heavy oils (e.g., coconut oil), which can clog pores. Alcohol-based products can over-dry and irritate the skin, worsening acne. Fragrances and sulfates might trigger irritation and allergic reactions. Instead, look for non-comedogenic, hypoallergenic products designed for sensitive skin.
Is Exfoliation Safe for Acne-Prone Skin?
Exfoliation can be safe for acne-prone skin, but it must be done gently and infrequently. Over-exfoliation can irritate and damage the skin barrier, worsening acne. Use mild chemical exfoliants like salicylic acid over harsh scrubs. Limit exfoliation to once or twice a week to avoid irritation.
Can Acne-Prone Skin Benefit from Facials?
Yes, acne-prone skin can benefit from facials, especially those tailored for sensitive skin. Professional facials can provide deep cleansing, exfoliation, and extraction, helping to clear clogged pores and reduce inflammation. However, choosing a gentle treatment and an experienced esthetician is crucial to avoid aggravating the skin.
How to Identify Non-Comedogenic Products for Acne-Prone Skin?
To identify non-comedogenic products for acne-prone skin, look for labels stating "non-comedogenic," "oil-free," or "won't clog pores." These products are formulated to not block pores. It's also helpful to review ingredient lists for known pore-clogging substances and choose products with a lighter, gel-based consistency.
How to Calm Redness in Acne-Prone Skin?
To calm redness in acne-prone skin, use skincare products containing soothing ingredients like aloe vera, green tea, and chamomile. Avoid harsh chemicals and scrubs, which can aggravate redness. Also, applying a cool compress and using over-the-counter anti-inflammatory creams can reduce redness. Gentle cleansing and moisturizing are essential for maintaining skin health.
Can Dehydration Affect Acne-Prone Skin?
Yes, dehydration can affect acne-prone skin. Lack of adequate hydration can lead to dryness, prompting the skin to produce more oil to compensate, which can exacerbate acne. Additionally, dehydrated skin has a compromised barrier function, making it more susceptible to irritation and inflammation, potentially worsening acne conditions.
Can Acne-Prone Skin Clear Up Naturally Over Time?
Acne-prone skin can clear up naturally over time, especially as hormonal fluctuations stabilize with age. However, the timeframe varies for each individual and depends on factors like genetics, lifestyle, and skin care habits. Maintaining a healthy diet, proper skincare routine, and stress management can aid in natural improvement.
What Role Do Genetics Play in Acne-Prone Skin?
Genetics play a significant role in acne-prone skin. If parents had acne, there's a higher likelihood of developing it, due to inherited tendencies like excessive sebum production and skin cell turnover rates. Genetic factors also influence skin's sensitivity to hormonal changes, diet, and environmental triggers that can exacerbate acne.
Can Diet Influence Fungal Acne?
Diet can influence fungal acne, as high-sugar and carbohydrate-rich diets may exacerbate it. These foods can alter the skin's yeast balance, promoting fungal growth. A balanced diet, low in processed sugars and high in nutrients, can help maintain a healthy skin microbiome, potentially reducing fungal acne outbreaks.
Is Fungal Acne Contagious?
Fungal acne, caused by an overgrowth of yeast naturally present on the skin, is not contagious. Unlike bacterial acne, it doesn't spread through skin-to-skin contact or sharing personal items. It's a reaction to an internal imbalance in the skin's microbiome, often exacerbated by warm, moist environments.
How Long Does Fungal Acne Last?
The duration of fungal acne varies, typically lasting weeks to months without treatment. With appropriate antifungal medications and skincare adjustments, such as using non-comedogenic and anti-fungal products, improvement can be seen in a few weeks. Persistent or severe cases may require longer treatment and consultation with a dermatologist.
How Can I Identify Fungal Acne?
Fungal acne appears as small, uniform, itchy red bumps, often on the chest, back, and arms, distinguishing it from bacterial acne. It may worsen with sweat and doesn't respond to typical acne treatments. A dermatologist can confirm it through examination and possibly a skin culture or microscopy.
What Is the Role of Yeast in Fungal Acne?
In fungal acne, yeast (specifically Malassezia) plays a central role. This yeast is part of the skin's normal flora but can overgrow under certain conditions, like humid environments and imbalanced skin microbiomes, leading to inflammation and acne-like breakouts. Fungal acne occurs when this yeast disrupts hair follicles.
Are Oils Bad for Fungal Acne?
Many oils can be bad for fungal acne, as they provide a food source for the yeast causing the condition. Oils like olive or coconut oil can exacerbate fungal acne. It's recommended to use non-comedogenic and anti-fungal oils, like tea tree oil, which don't feed the yeast.
What Is the Impact of Pollution on Acne-Prone Skin?
Pollution can significantly impact acne-prone skin. Pollutants like smog, dust, & smoke contain toxins that can clog pores & increase inflammation, exacerbating acne. They also contribute to oxidative stress, damaging skin cells & accelerating aging. Regular cleansing & using antioxidants in skincare can help mitigate these effects.
Are Spot Treatments Effective for Acne-Prone Skin?
Spot treatments can be effective for acne-prone skin, targeting specific blemishes with concentrated ingredients like salicylic acid or benzoyl peroxide. They help reduce inflammation & bacteria, speeding up healing. However, they're part of a broader skincare routine & not a standalone solution for widespread or severe acne.
How Does Sun Exposure Affect Acne-Prone Skin?
Sun exposure can initially seem beneficial for acne-prone skin, as it dries out pimples & masks redness. However, it can worsen acne long-term by increasing skin cell turnover, leading to clogged pores. Additionally, UV rays can damage skin & exacerbate inflammation. Sunscreen is vital to protect & prevent aggravation.
What Is Fungal Acne?
Fungal acne, medically known as Pityrosporum folliculitis, is caused by an overgrowth of yeast (a type of fungus) in hair follicles. Unlike traditional acne, it's characterized by small, uniform pimples, often itchy, commonly on the chest, back, & arms. It requires antifungal treatments, differing from bacterial acne treatments.
What Causes Fungal Acne?
Fungal acne is caused by an overgrowth of Malassezia yeast, naturally present on the skin. Factors contributing to this imbalance include humid environments, excessive sweating, tight clothing, a weakened immune system, antibiotic use (which disrupts skin flora), & oily skin. It's not caused by poor hygiene.
Can Fungal Acne Be Prevented?
Preventing fungal acne involves controlling factors that encourage yeast growth. Keep skin dry & clean, especially after sweating. Wear loose, breathable clothing. Use non-comedogenic, oil-free skincare products. Avoid prolonged antibiotic use when possible. Incorporating anti-fungal products into your routine can also help, especially in humid climates.
How Can You Reduce Inflammation in Acne-Prone Skin?
To reduce inflammation in acne-prone skin, gently cleanse twice daily with a mild, non-comedogenic cleanser. Apply topical treatments containing salicylic acid or benzoyl peroxide. Avoid harsh exfoliants and picking at the skin. Use oil-free, non-irritating moisturizers and sunscreens. Consult a dermatologist for persistent or severe cases.
How Can You Prevent Acne Flare-Ups?
To prevent acne flare-ups, maintain a consistent skincare routine with gentle, non-comedogenic products. Regularly wash your face, especially after sweating. Avoid touching your face and picking at blemishes. Manage stress, eat a balanced diet, and stay hydrated. Use oil-free makeup and remove it before sleeping. Consult a dermatologist if needed.
What Are Effective Treatments for Acne Scars?
Effective treatments for acne scars include laser therapy, microneedling, chemical peels, and dermal fillers. Topical retinoids and hydroquinone can also help. It's essential to protect scars from sun exposure. Consult a dermatologist to determine the best treatment plan based on scar type and skin condition.
Can Hormonal Changes Affect Acne-Prone Skin?
Yes, hormonal changes can significantly affect acne-prone skin. Fluctuations, particularly in androgens, can increase oil production, leading to clogged pores and breakouts. This is common during puberty, menstrual cycles, pregnancy, and menopause, or due to conditions like polycystic ovary syndrome (PCOS). Hormone therapy may be beneficial in some cases.
How to Select Makeup for Acne-Prone Skin?
To select makeup for acne-prone skin, choose non-comedogenic products labeled as "oil-free" or "water-based." Look for ingredients like salicylic acid or benzoyl peroxide for added acne-fighting benefits. Prioritize mineral-based foundations and avoid heavy, pore-clogging formulas. Always cleanse your face before and after wearing makeup to prevent breakouts.
How Can Diet Influence Acne-Prone Skin?
Diet can influence acne-prone skin by affecting hormone levels and inflammation. High-glycemic foods, dairy, and sugary items may exacerbate acne due to insulin spikes and increased sebum production. A diet rich in fruits, vegetables, and whole grains can help reduce inflammation and promote clearer skin. Staying hydrated is also essential.
What Treatments Are Effective for Fungal Acne?
Effective treatments for fungal acne include antifungal creams or shampoos containing ketoconazole or ciclopirox. Oral antifungal medications like fluconazole may be prescribed for severe cases. It's important to avoid oil-based skincare products and maintain a clean, dry skin environment to prevent further irritation or spread. Regular dermatologist consultations are recommended.
How to Manage Oily Acne-Prone Skin?
To manage oily acne-prone skin, cleanse twice daily with a gentle, non-comedogenic cleanser. Use oil-free, water-based moisturizers and makeup. Exfoliate weekly to remove dead skin cells. Apply a salicylic acid or benzoyl peroxide treatment to target acne. Avoid touching your face, and always remove makeup before sleeping.
Why Is My Fungal Acne Not Improving?
Fungal acne may not improve if misdiagnosed or treated with regular acne products, which can worsen it. Ensure proper diagnosis, use antifungal treatments like ketoconazole, avoid occlusive skincare, and maintain a routine. Consult a dermatologist for targeted advice and possibly oral antifungals if topical treatments fail.
Can Exfoliation Help Treat Fungal Acne?
Exfoliation can help treat fungal acne by removing dead skin cells that clog pores and exacerbate the condition. However, it should be gentle and not overdone, as harsh exfoliation can irritate the skin and worsen fungal infections. Always combine with antifungal treatments for best results.
What Lifestyle Changes Can Help Acne-Prone Skin?
For acne-prone skin, lifestyle changes can be beneficial. Include a balanced diet rich in fruits, vegetables, & lean proteins. Reduce dairy & high glycemic foods. Stay hydrated, maintain good hygiene, avoid excessive touching of the face, manage stress, & ensure adequate sleep. Also, use non-comedogenic skincare products.